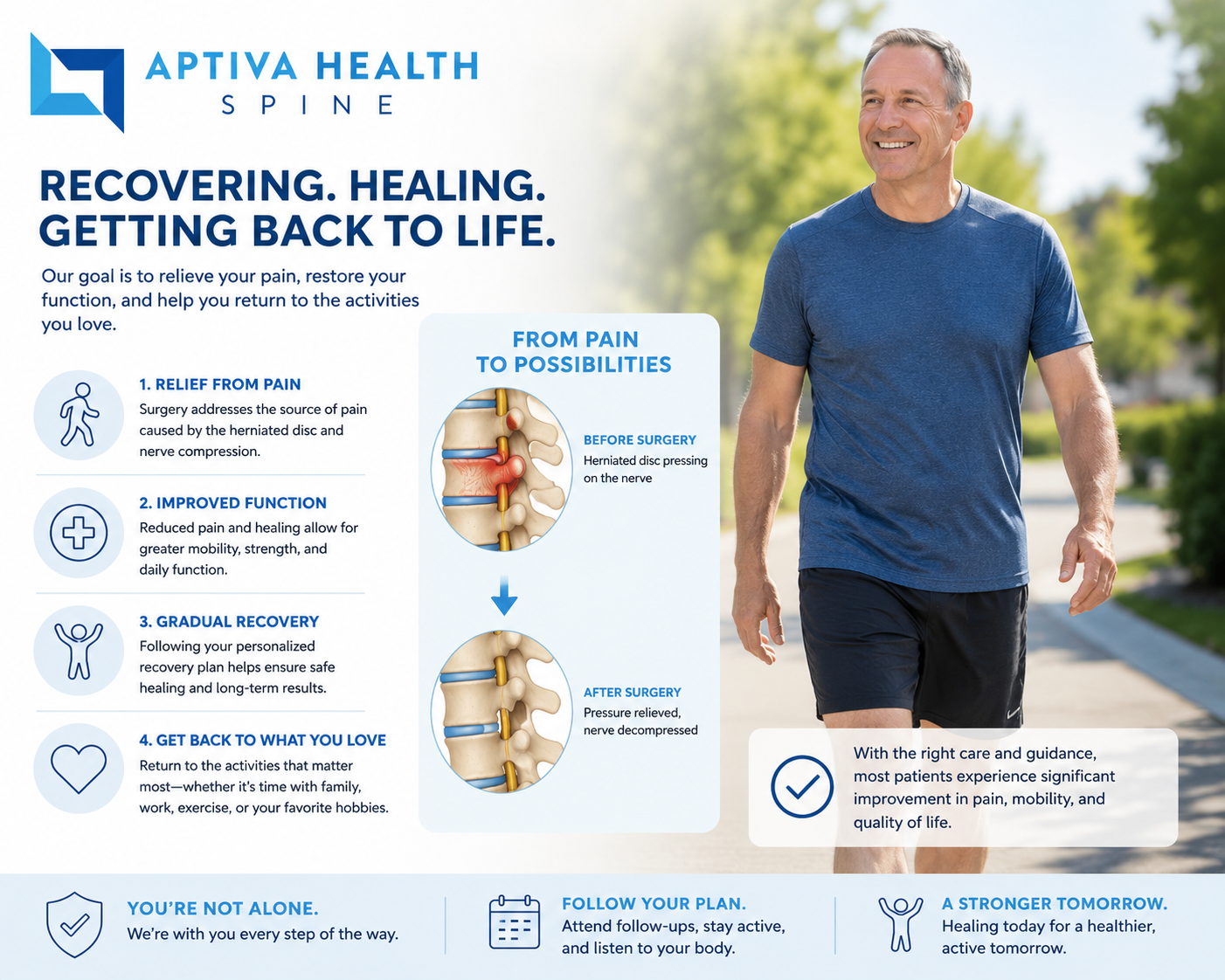
Herniated Disc Treatment
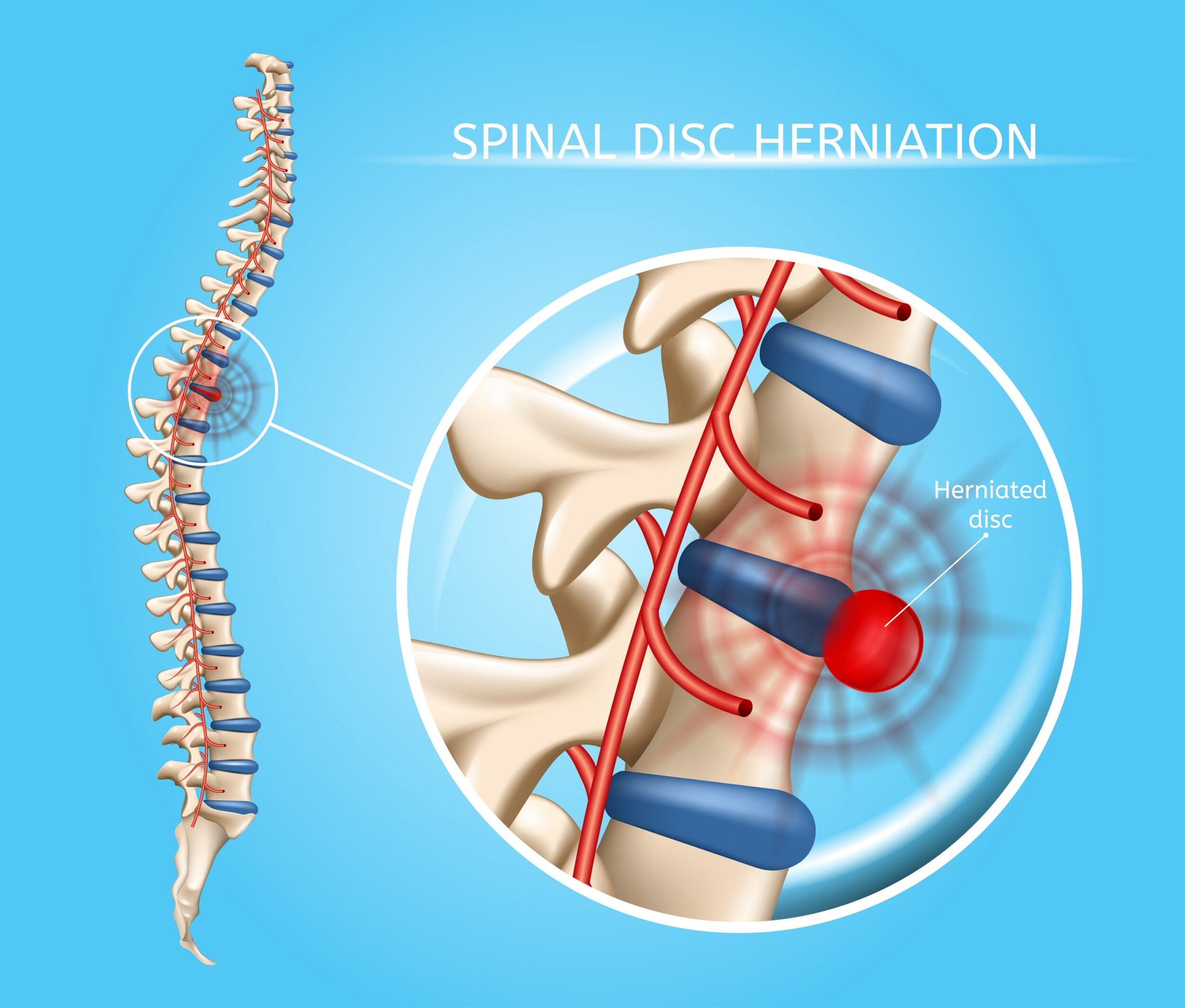
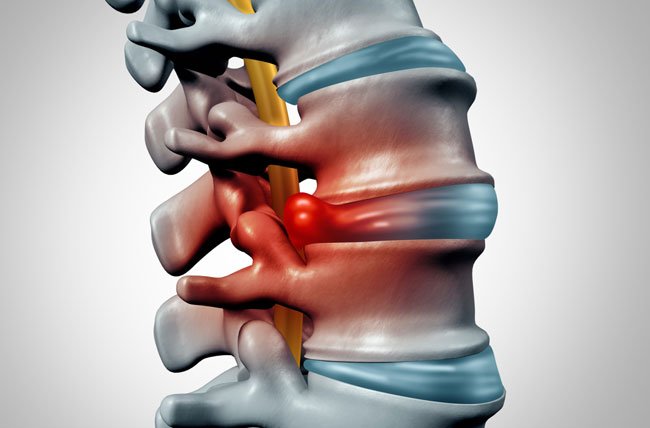
Disc Herniation
A herniated disc happens when the soft inner core of a spinal disc pushes through its tough outer wall and presses on a nearby nerve, causing pain, numbness, weakness, or tingling in the back, neck, arm, or leg. At Aptiva Health, three board-certified orthopedic spine surgeons — Dr. Michael Casnellie, Dr. Jaideep Chunduri, and Dr. David McConda — and our double board-certified pain management physician Dr. Steven Ganzel evaluate suspected herniated discs at every Aptiva location across Kentucky and Indiana. Most patients are seen within 24 hours, imaged on-site with our advanced MRI, and start physical therapy or injection therapy within the same week — so you get back to your life as fast as possible.
Medically reviewed by Michael Casnellie, MD, Jaideep Chunduri, MD, David McConda, MD, and Steven Ganzel, DO. Last reviewed: May 2026.
The Aptiva Difference
Why patients with disc herniation choose Aptiva Health:
Most patients evaluated within 24 hours of contacting us
On-site MRI (Phillips Panorama Open MRI and Siemens Espree wide-bore) — most patients imaged the same week, often the same day
Same-week start on physical therapy or fluoroscopy-guided injections
Three board-certified orthopedic spine surgeons + a double board-certified pain management physician + an in-house physical therapy team — all under one roof
Treated at every Aptiva location across Kentucky and Indiana
Same-day and walk-in appointments — no primary care referral required
Schedule your appointment today!
What is a herniated disc?
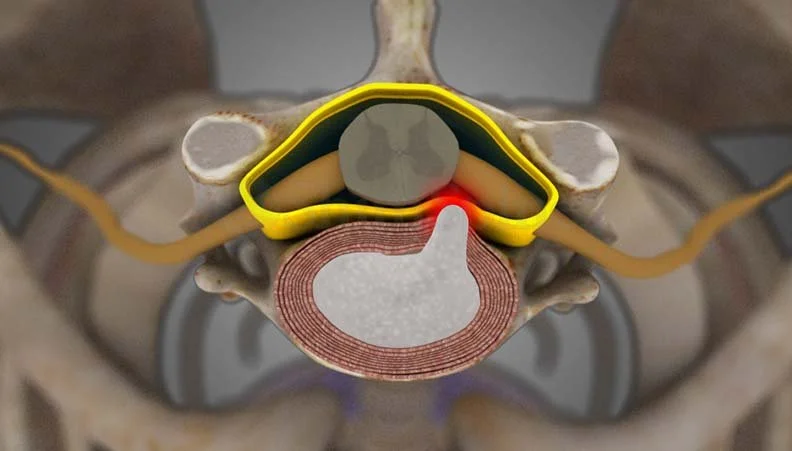
The discs in your spine sit between each pair of vertebrae and act as shock absorbers. Each disc has a tough outer ring (the annulus fibrosus) and a soft, gel-like center (the nucleus pulposus). A disc becomes herniated when that soft inner material pushes through a tear or weak spot in the outer ring and presses against a nearby spinal nerve.
You may also hear a herniated disc called a slipped disc, ruptured disc, bulging disc, or pinched nerve. These terms describe slightly different things clinically, but patients use them interchangeably and so do most search engines.
Disc herniations can occur anywhere along the spine, but they happen most commonly in two locations:
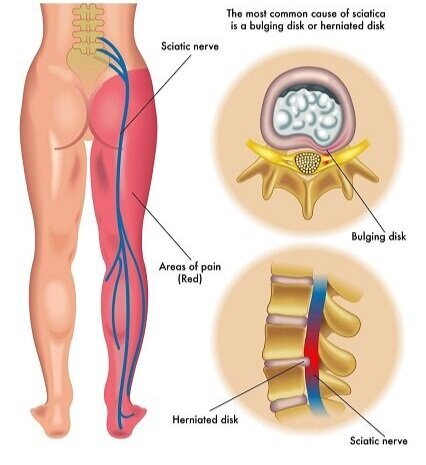
Lumbar spine (lower back) — the most common location. Lumbar disc herniation typically causes lower back pain that radiates into the buttock and down one leg, a symptom pattern called sciatica.
Cervical spine (neck) — the second most common location. Cervical disc herniation typically causes neck pain that radiates into the shoulder, arm, or hand, a symptom pattern called cervical radiculopathy.
Disc herniations in the thoracic spine (mid-back) are uncommon but do occur, usually after trauma.
What are the symptoms of a herniated disc?
Symptoms depend on where the herniation is and which nerve is being compressed. Many people have a small disc herniation on imaging without any symptoms at all. The herniations that cause pain are the ones pressing on a nerve.
Lumbar (lowback) disc herniation symptoms:
Sharp, burning, or electric pain that radiates from the lower back into the buttock and down one leg (sciatica).
Numbness or tingling in the leg, calf, foot, or toes on the affected side.
Weakness in the leg or foot — for example, difficulty lifting the foot or rising on tiptoes.
Pain that worsens when sitting, coughing, sneezing, or bending forward.
Lower back pain that may or may not be the dominant symptom.
Cervical (neck) disc herniation symptoms:
Neck pain or stiffness, often on one side.
Sharp, burning, or electric pain that radiates from the neck into the shoulder, arm, forearm, or hand.
Numbness or tingling in the shoulder, arm, hand, or specific fingers.
Weakness in the arm, hand, or grip strength.
Pain that worsens with certain neck positions, especially looking up or turning the head toward the affected side.
Red-flag symptoms - get to an emergency room immediately
These symptoms can indicate spinal cord compression or cauda equina syndrome, both of which are surgical emergencies:
New loss of bladder or bowel control.
Numbness in the inner thighs, groin, or buttocks (saddle anesthesia).
Sudden, severe weakness in both arms or both legs.
Progressive difficulty walking or loss of fine motor coordination in the hands.
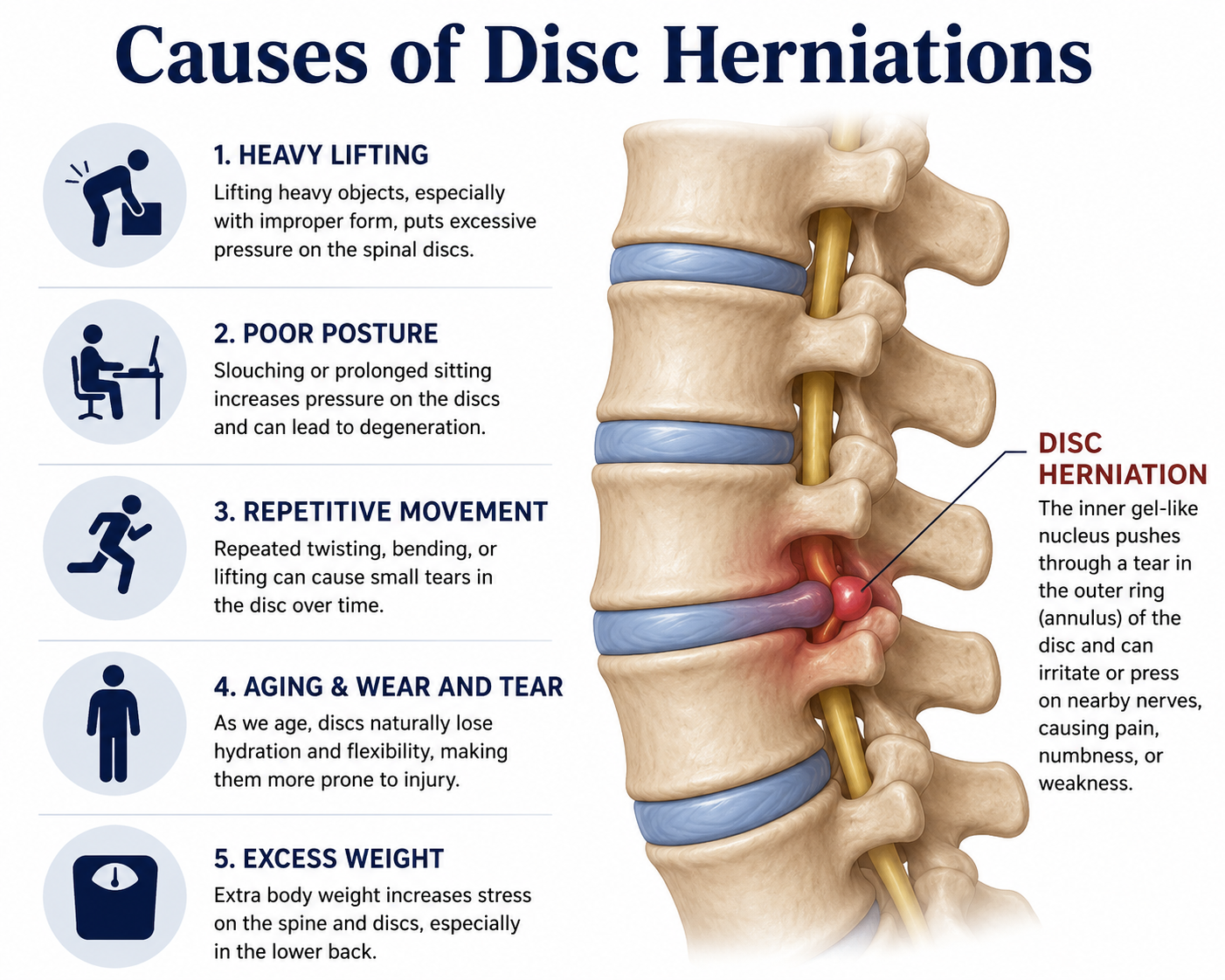
What causes a herniated disc?
Most disc herniations are caused by a combination of age-related disc wear and a triggering event. The discs lose water and elasticity as we age, and the outer ring weakens — making it easier for an everyday motion to cause a herniation that would not have happened a decade earlier.
Common contributors:
Age-related disc degeneration — the most common underlying factor; disc herniations are most common between ages 30 and 50.
Lifting injuries — especially lifting heavy objects with poor mechanics or while twisting.
Sudden trauma — falls, motor-vehicle accidents, or sports injuries.
Repetitive bending, twisting, or vibration — common in trades, manufacturing, transportation, and certain athletic activities.
Smoking — accelerates disc degeneration.
Genetics — disc problems often run in families.
Excess body weight — adds mechanical stress to the lumbar discs.
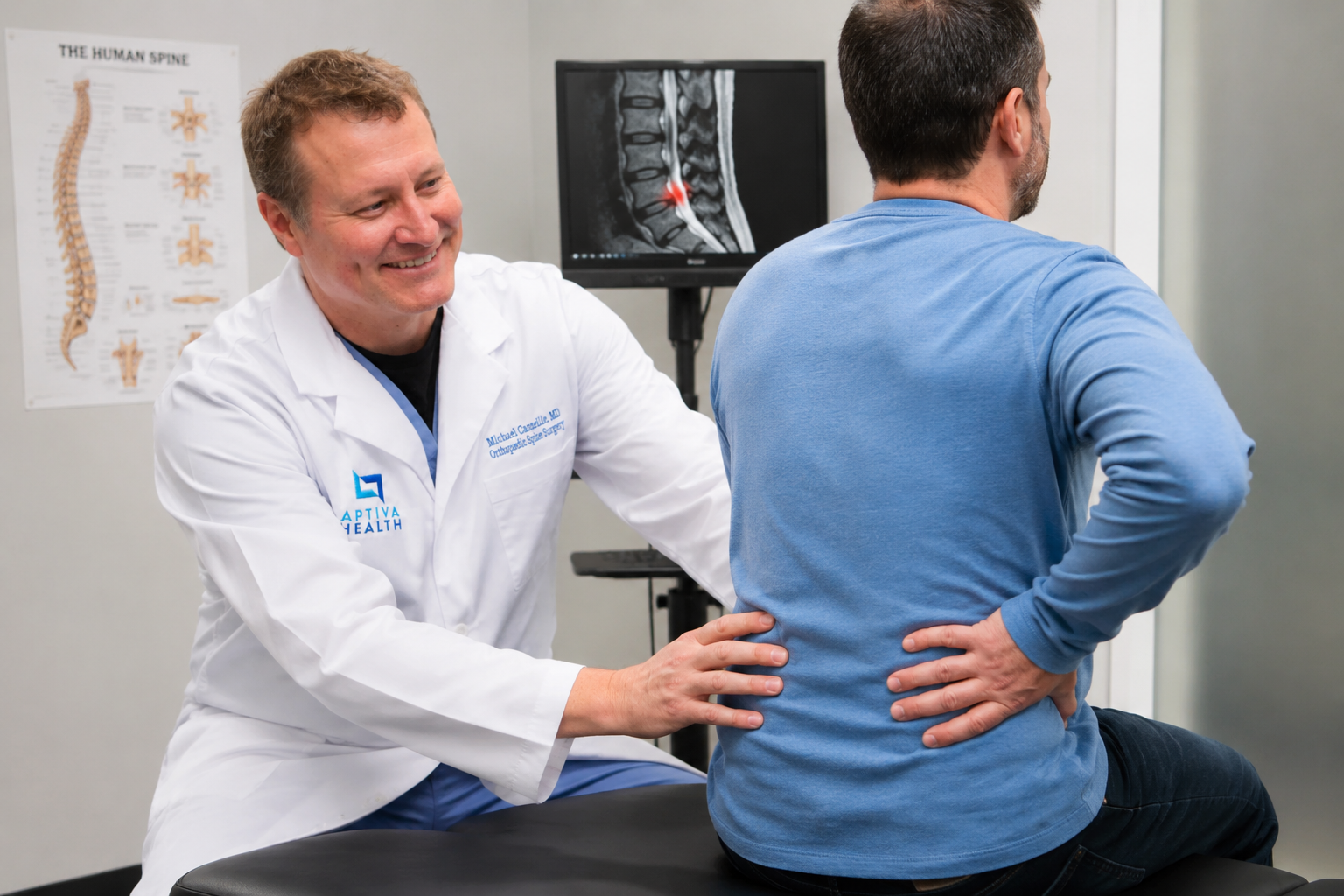
How is a herniated disc diagnosed at Aptiva Health?
Precision diagnosis is the second pillar of how Aptiva Health treats disc herniation. A correct diagnosis tells us exactly which disc is herniated, exactly which nerve is involved, and exactly how severely — and that is what makes a custom-tailored treatment plan possible.
Your evaluation typically includes:
A focused medical history. Your provider will ask exactly when the pain started, what triggered it, where it radiates, what makes it better or worse, what activities or postures aggravate it, and your full neurologic symptom map.
A targeted physical and neurologic exam. This includes the straight-leg raise test (for lumbar herniations), Spurling's test (for cervical herniations), reflex testing, sensation mapping, and strength testing of specific muscle groups. Together these often pinpoint the exact nerve root involved before any imaging is ordered.
Advanced on-site imaging. This is where Aptiva is set up differently from most competitors. We have two on-site MRI systems — a Phillips Panorama High Field Open MRI (available in Louisville) for patients who prefer or require an open-bore experience, and a Siemens Espree wide-bore (70 cm) MRI for high-resolution diagnostic imaging (available in Louisville, Lexington, and northern Kentucky). MRI is the gold standard for visualizing disc herniations because it shows the disc, the nerve, and the surrounding soft tissue at the same time. Most Aptiva patients are imaged the same week as their first visit, often the same day, eliminating the multi-week delay that scheduling at an outside imaging center can introduce.
X-ray when indicated. Aptiva offers digital X-ray on-site at every clinic location, so bony alignment, fractures, spondylolisthesis, and disc-space narrowing can be evaluated in the same visit.
Selective diagnostic injections when needed. In complex cases where imaging is ambiguous or shows multiple potential pain generators, Dr. Steven Ganzel can perform a fluoroscopy-guided selective nerve root block — a diagnostic injection that confirms which specific nerve is generating your symptoms.
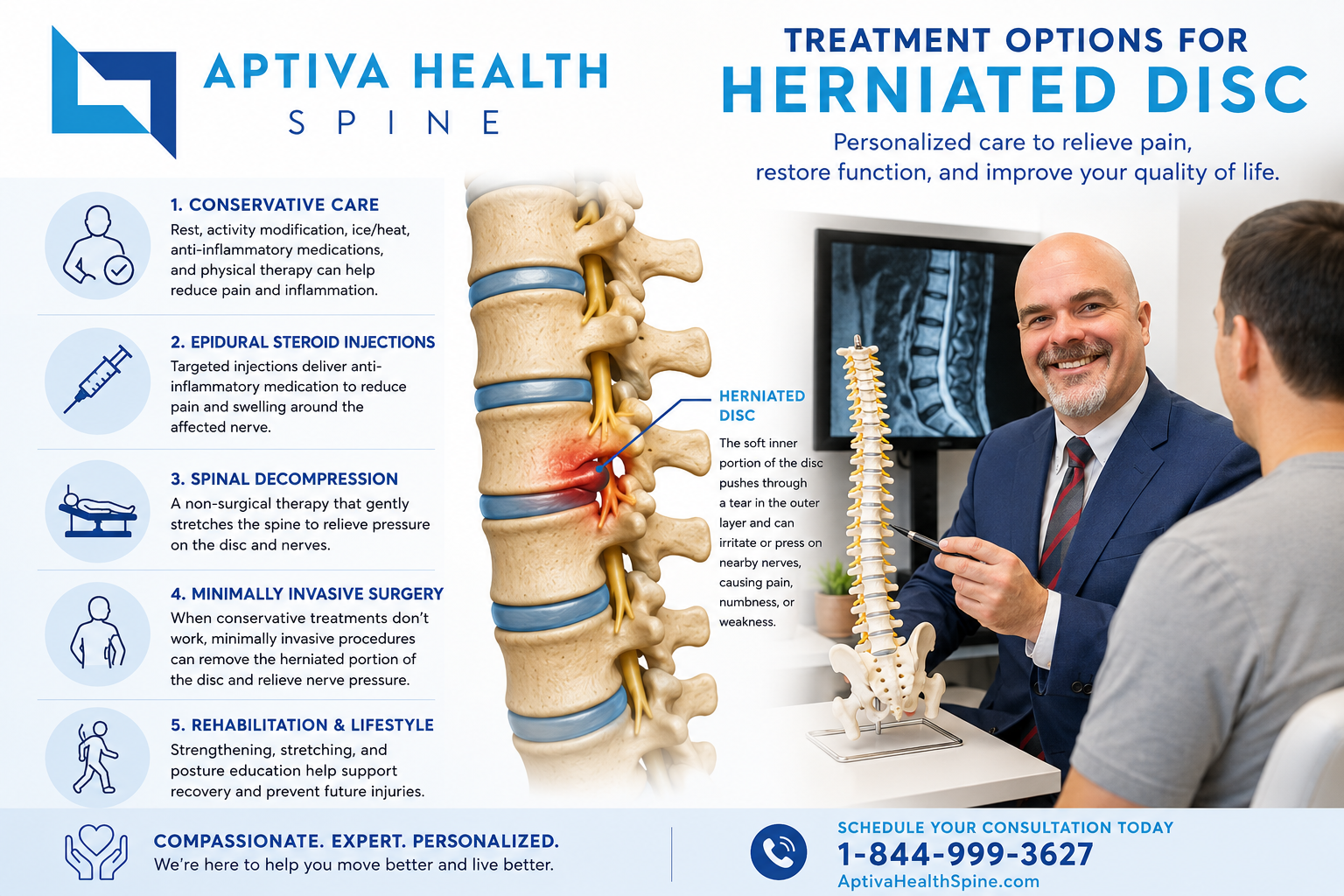
How is a herniated disc treated?
A custom-tailored treatment plan is the third pillar. Most herniated discs improve without surgery — the body reabsorbs disc material and inflammation settles over weeks to months. The Aptiva Health spine team uses a stepped-care approach, starting with the least-invasive options that match your specific cause and severity, and progressing to more advanced interventions only when needed.
Non-surgical treatement for a herniated disc
Most patients start here, and most patients improve here.
Targeted physical therapy — Aptiva's in-house physical therapy team uses spine-specific exercises, manual therapy, dry needling, McKenzie protocols, and traction to reduce nerve irritation and rebuild the muscles that support the spine. Patients typically begin physical therapy within the same week as their initial evaluation.
Activity modification — short-term avoidance of the postures and movements that aggravate your specific herniation pattern, while you build the strength and conditioning to safely return to them.
Anti-inflammatory medication — NSAIDs (ibuprofen, naproxen) for inflammation around the nerve root.
Short-course oral steroids — for moderate to severe acute symptoms.
Muscle relaxants — short-term use to break the cycle of muscle spasm that often accompanies a fresh disc herniation.
Heat and cold therapy — alternating ice (for inflammation) and heat (for muscle relaxation).
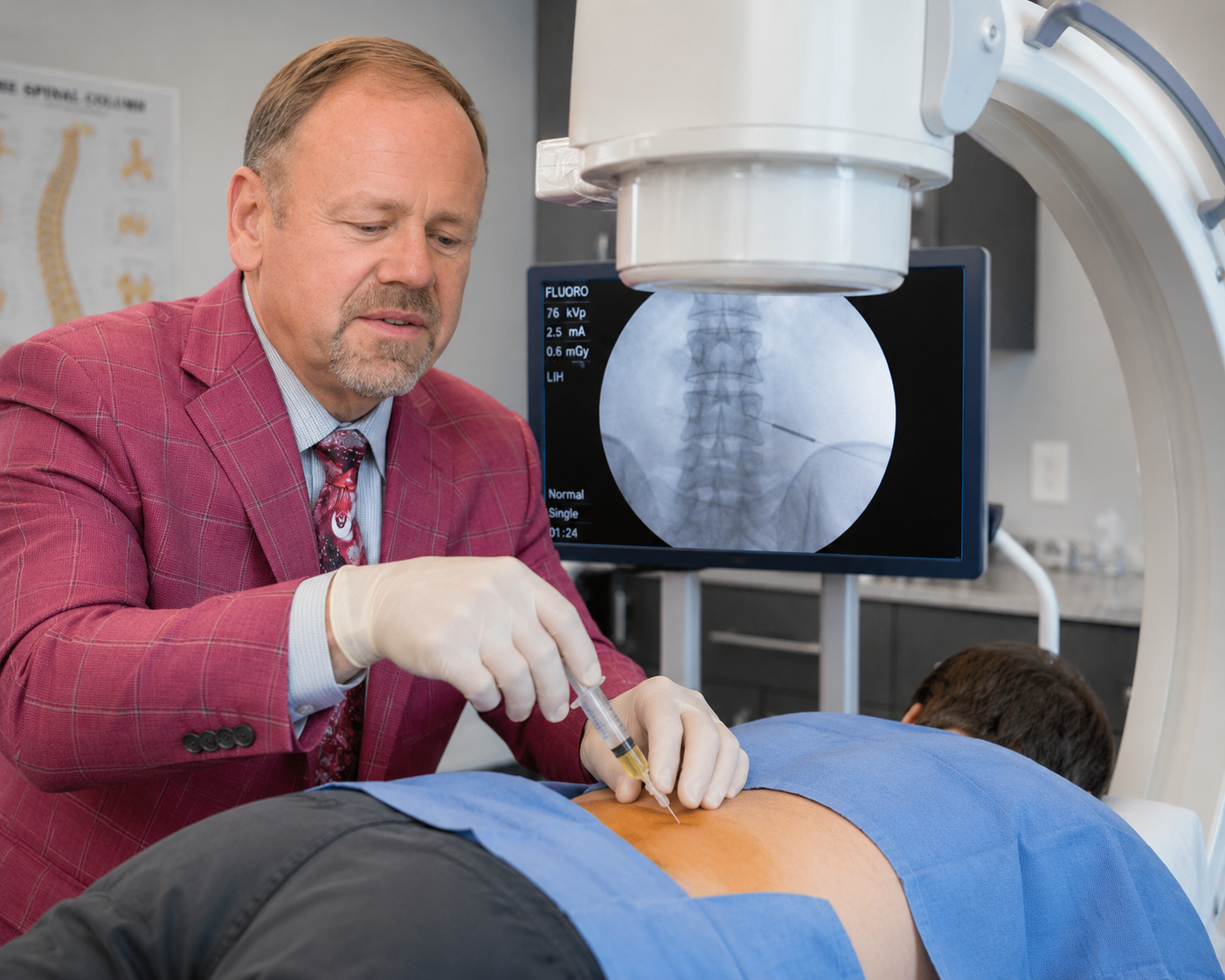
Injection treatments for herniated disc
When physical therapy and oral medication are not enough, fluoroscopy-guided injections — performed under live X-ray by Dr. Steven Ganzel, our double board-certified Physical Medicine & Rehabilitation and Interventional Pain Management physician — provide both diagnostic and therapeutic value. Most patients can begin injection therapy within the same week as diagnosis.
Lumbar epidural steroid injection may be performed utilizing a spinal needle under X-ray guidance (through the use of a c-arm) to direct the medication to the exact level of the disc herniation for more moderate to severe symptoms.
Cervical epidural steroid injection — the same approach for nerve roots in the neck.
Selective nerve root block — a targeted injection used both diagnostically (to confirm which nerve is responsible) and therapeutically.
Facet joint injection — when the small joints between vertebrae are also contributing to the pain pattern.
Minimally Invasive Surgery for Herniated Disc
Surgery is considered when conservative care has not improved symptoms after six to twelve weeks, when there is progressive neurologic weakness, or when the disc herniation is causing severe symptoms that are clearly not going to resolve with time. All three Aptiva Health spine surgeons — Dr. Michael Casnellie, Dr. Jaideep Chunduri, and Dr. David McConda — are board-certified orthopedic spine surgeons specializing in minimally invasive techniques that use smaller incisions and muscle-splitting (rather than muscle-cutting) approaches to speed recovery.
Common surgical options for lumbar disc herniation:
Microdiscectomy — Aptiva's most common spine surgery for lumbar disc herniation. Performed by Dr. Casnellie, Dr. Chunduri and Dr. McConda using a 1–2 cm midline incision, an operating microscope, and microsurgical instruments. The herniated portion of the disc is removed; the rest of the disc and the surrounding muscles are preserved. Most patients return home the same day.
Laminotomy / laminectomy with discectomy — when bone overgrowth or stenosis is contributing alongside the herniation.
Minimally invasive lumbar fusion (MAS® TLIF) — when disc herniation occurs alongside instability or spondylolisthesis. Aptiva spine surgeons specialize in the MAS® TLIF approach, which uses a muscle-splitting (rather than muscle-cutting) technique to reduce blood loss, scarring, and recovery time compared with traditional open lumbar fusion.
Common surgical options for cervical disc herniation:
Cervical disc replacement (cervical disc arthroplasty) — replaces a damaged cervical disc with an artificial disc designed to preserve motion at the treated level, reducing the long-term stress on adjacent levels. Dr. Michael Casnellie performed the first cervical disc arthroplasty in the region and continues to offer this advanced motion-preserving option for appropriate candidates.
Anterior cervical discectomy and fusion (ACDF) — the most common surgery for cervical disc herniation. The damaged disc is removed through a small incision in the front of the neck and the two vertebrae are fused together.
Posterior cervical foraminotomy — for select cases where the herniation is laterally located, this minimally invasive option preserves the disc entirely.
Recovery from a herniated disc
Recovery time depends on whether your treatment is non-surgical or surgical, and on the size and location of the herniation. Typical timelines:
Most non-surgical herniated discs improve significantly within 6 to 12 weeks of consistent physical therapy, activity modification, and (when needed) two to three epidural steroid injections.
After microdiscectomy, most patients return to desk work in 2 weeks, light physical activity in 4 to 6 weeks, and full activity in 8 to 12 weeks.
After cervical disc replacement or ACDF, most patients return to desk work in 1 to 2 weeks, with progressive return to full activity over 3 months as the artificial disc settles or the bone heals.
After minimally invasive lumbar fusion (MAS® TLIF), recovery takes 3 to 6 months as bone fusion progresses, with most patients returning to full activity by 6 months.
When should you see a doctor for a herniated disc?
Many people have small disc herniations they never notice. The herniations that need evaluation are the ones causing symptoms. See a spine specialist if you have:
Pain that radiates from the lower back into the leg, or from the neck into the arm.
Numbness, tingling, or weakness in an arm, hand, leg, or foot.
Pain that has not improved after one to two weeks of self-care.
Pain severe enough to interfere with sleep, work, or daily activity.
Pain that began after an injury, fall, motor-vehicle accident, or work-related incident.
Get to an emergency room immediately for new bladder or bowel changes, saddle anesthesia, or sudden severe weakness in both legs or both arms.
For non-emergency disc herniation symptoms, Aptiva Health offers immediate appointments at every clinic location, with most patients evaluated within 24 hours of contacting us. Free 24/7 virtual access to an orthopedic provider is also available through the HURT! app.
Why choose Aptiva Health for herniated disc treatment?
Most patients with disc herniation end up coordinating care across three or four separate practices: a primary care office for the referral, a spine clinic for the evaluation, an outside imaging center for the MRI, a pain clinic for the injection, and a separate physical therapy practice for rehab — each with its own scheduling, its own paperwork, and its own waiting time. Aptiva Health is built differently. The full continuum of disc herniation care lives under one roof.
The Aptiva winning formula:
Immediate access to specialized care.
Most patients are evaluated within 24 hours of contacting Aptiva Health.
Same-day and walk-in spine appointments at every location.
No primary care referral required.
Free 24/7 virtual access through the HURT! app.
Precision diagnosis through advanced on-site imaging.
On-site Phillips Panorama High Field Open MRI and Siemens Espree wide-bore (70 cm) MRI.
On-site digital X-ray at every location.
Most patients imaged the same week as their first visit, often the same day.
Diagnostic selective nerve root blocks available when imaging is ambiguous.
Custom-tailored treatment plans, all under one roof.
Three board-certified orthopedic spine surgeons — Dr. Michael Casnellie, Dr. Jaideep Chunduri, and Dr. David McConda — for surgical evaluation and minimally invasive surgery when needed.
A double board-certified pain management physician — Dr. Steven Ganzel — for fluoroscopy-guided injections.
In-house physical therapy with dry needling, manual therapy, McKenzie protocols, and post-surgical rehab.
Same-week start on physical therapy or injection therapy after diagnosis.
Cervical disc replacement available — Dr. Casnellie performed the region's first cervical disc arthroplasty.
Practical and accessible.
Disc herniation evaluated and treated at every Aptiva Health location across Kentucky and Indiana.
In-network with Anthem, Aetna, Cigna, Humana, United Healthcare, Medicare, Kentucky Medicaid (orthopedics), VA, and Humana Military.
Transparent self-pay pricing for patients without insurance.
Where we treat disc herniations
Aptiva Health treats disc herniation at every clinic location across Kentucky and Indiana — same spine team, same advanced imaging, same same-week access:
Spine Center of Excellence: 3615 Newburg Road, Louisville, KY 40218
Louisville - East: 10100 Linn Station Road, Suite 1A, Louisville, KY 40223
Concussion & Sports Medicine Institute: 3611 Newburg Road, Louisville, KY 40218
Elizabethtown: 529 Westport Road, Suite 2, Elizabethtown, KY 42701
Indianapolis: 6801 Gray Road, Indianapolis, IN 46237
Louisville - Downtown: 300 South 13th Street, Louisville, KY 40203
Louisville - Middletown: 401 N English Station Road, Suite 1A, Louisville, KY 40223
Lexington Physical Therapy: 152 W Tiverton Way, Suite 180, Lexington, KY 40503
Mount Washington: 737 N Hwy 31e Byp, Suite 2, Mt. Washington, KY 40047
Northern Kentucky: 2093 Medical Arts Drive, Hebron, KY 41048
Frequently asked questions about herniated discs
Can a herniated disc heal on its own?
Yes. Some herniated discs improve on their own over 6 to 12 weeks as the body reabsorbs the herniated disc material and inflammation settles. Most patients recover fully without surgery — particularly when they pair time with targeted physical therapy and, when needed, an epidural steroid injection. The herniated discs that do not heal on their own typically have larger fragments, more severe nerve compression, or accompanying anatomic problems like spondylolisthesis.
What is the fastest way to recover from a herniated disc?
The fastest recoveries follow a structured plan: an evaluation by a spine specialist within the first week or two, an MRI to confirm exactly which disc and which nerve are involved, immediate start of targeted physical therapy, an early epidural steroid injection if severe pain is interfering with rehab, and modified activity in the meantime. At Aptiva Health, most patients are evaluated within 24 hours, imaged on-site within the same week, and started on physical therapy or injections within that same week — which compresses the typical recovery timeline significantly.
What is the difference between a herniated disc and a bulging disc?
A bulging disc is a disc whose entire outer ring extends beyond its normal boundary, like a tire that has lost its shape. A herniated disc has a focal tear in the outer ring through which inner disc material has pushed outward. Bulging discs are very common and often cause no symptoms; herniated discs are more likely to compress a nerve and cause pain or weakness. The treatment principles are similar, but herniations are more likely to require injections or surgery.
How is a herniated disc diagnosed?
Diagnosis combines a detailed history, a focused neurologic exam (including straight-leg raise for the lumbar spine and Spurling's test for the cervical spine), and MRI imaging. MRI is the gold standard because it shows the disc, the nerve, and the surrounding soft tissue at the same time. Aptiva Health offers on-site MRI with both Phillips Panorama Open MRI and Siemens Espree wide-bore systems, so most patients are imaged within the same week as their first visit. X-rays may also be ordered to rule out fractures, spondylolisthesis, or disc-space narrowing.
Do I need surgery for a herniated disc?
Most patients with a herniated disc will not need surgery. Surgery is considered when conservative care — physical therapy, anti-inflammatory medication, and at least one epidural steroid injection — has not improved symptoms after six to twelve weeks, when there is progressive neurologic weakness, or when the herniation is causing severe symptoms unlikely to resolve with time. When surgery is needed, Aptiva spine surgeons perform minimally invasive options including microdiscectomy, cervical disc replacement, and minimally invasive lumbar fusion that allow most patients to return home the same day.
How long does a herniated disc take to heal?
Acute herniated disc symptoms can improve over 6 to 12 weeks with conservative care. Imaging changes can lag — the disc may continue to shrink for 6 to 12 months even after symptoms have resolved. Patients who have surgery typically return to desk work in 1 to 2 weeks, light activity in 4 to 6 weeks, and full activity in 2 to 3 months.
What does a herniated disc feel like?
A herniated disc most often causes radiating pain — pain that travels from the spine into a limb. A lumbar herniation typically causes lower back pain that radiates into the buttock and down one leg, often with numbness, tingling, or weakness in the leg or foot. A cervical herniation typically causes neck pain that radiates into the shoulder, arm, or hand, often with numbness, tingling, or weakness in the affected arm or specific fingers. Pain is usually worse with certain positions — sitting and bending forward for lumbar herniations, looking up or turning the head for cervical herniations.
Can a herniated disc cause permanent nerve damage?
Some herniated discs may not cause permanent damage. However, severe or prolonged nerve compression can produce lasting numbness, weakness, or loss of reflex even after the disc itself has been treated. This is why progressive weakness is considered a reason to escalate treatment quickly, including consideration of surgery. Red-flag symptoms — bladder or bowel changes, saddle numbness, or sudden severe weakness in both limbs — are surgical emergencies and should be evaluated in an emergency room.
Is herniated disc treatment covered by insurance?
Yes. Evaluation, MRI imaging, physical therapy, epidural injections, and surgical treatment for herniated disc are covered by most commercial insurance plans, Medicare, and Kentucky Medicaid (for orthopedics). Aptiva Health is in-network with Anthem, Aetna, Cigna, Humana, United Healthcare, Medicare, Kentucky Medicaid for orthopedics, VA, and Humana Military, and offers transparent cash-pay pricing for patients without insurance.
How quickly can I be seen at Aptiva Health for a herniated disc?
Most patients with a suspected herniated disc are evaluated within 24 hours of contacting Aptiva Health. Immediate spine appointments are available at every Aptiva clinic location, including Louisville, Lexington, Northern Kentucky (Hebron), Elizabethtown, Mt. Washington, and our new Indianapolis location opening May 2026. The HURT! app provides free, 24/7 virtual access to an orthopedic provider for after-hours guidance.
Will Aptiva treat my herniated disc at every location?
Yes. Disc herniation is evaluated and treated at every Aptiva Health location. The same spine team — Dr. Michael Casnellie, Dr. Jaideep Chunduri, Dr. David McConda, Dr. Steven Ganzel, and our physical therapy team — covers every Aptiva clinic across Kentucky and Indiana, with on-site digital X-ray everywhere and on-site MRI in our Louisville, Lexington, and northern Kentucky imaging centers.
What kind of MRI does Aptiva use for herniated disc?
Aptiva Health uses two on-site MRI systems. Our Phillips Panorama High Field Open MRI offers a 360-degree panoramic viewing angle and a 160 cm-wide patient aperture — ideal for patients who feel claustrophobic in traditional closed MRIs or who require an open-bore design. Our Siemens Espree is a wide-bore (70 cm) high-field MRI for high-resolution diagnostic imaging. Most patients are imaged within the same week as their first Aptiva visit, often the same day.
Don't wait weeks to find out what's causing your back or neck pain. Aptiva Health's board-certified spine team can evaluate your symptoms within 24 hours, image you on-site that same week, and start treatment — physical therapy or injection therapy — before most other practices have even returned your call.