Auto Injury Treatment in Indianapolis
Car Accident Injury Care in Indianapolis
If you've been hurt in a car accident in Indiana, Aptiva Health can see you immediately. Our emergency medicine team, general medical practitioners, orthopedic surgeons, spine specialists, concussion team, pain management specialists, mental wellness providers, physical therapists, and advanced imaging centers work together across Indianapolis to ensure patients get the most comprehensive care possible in the event they are injured in a motor vehicle collision.
Why Aptiva Health for Auto Injury Care?
Integrated Health Care Model - Team Care Approach
Immediate Appointments Available for Patients
Convenient Indianapolis Location with Access to Advanced Imaging
Comprehensive Injury Care Specialists & Surgeons
Flexible Payment Options & Most Insurances Accepted
No Referral Required to Schedule an Appointment
Free 24/7 After-Hours Injury Triage Service
Schedule your appointment now!
Auto Injury-Related Data in Indianapolis - 2025
What do I do after a Car Accident in Indianapolis?
Most people who are injured in a car accident don't know where to go for medical care, and many delay the visit because they feel "okay" right after the crash. That delay can turn a treatable injury into a chronic one. Whiplash, concussion, and soft-tissue injuries often don't produce symptoms for 24 to 72 hours after impact, so the absence of pain at the scene is not reliable.
If you're not in life-threatening condition, an outpatient injury clinic like Aptiva Health is usually the right place to be evaluated within 72 hours. Here's the order we recommend:
Call 911 if anyone is seriously hurt or unconscious. Then go to the nearest emergency room. ERs are designed for life-threatening trauma — fractures, head bleeds, internal injuries.
If you're walking, talking, and oriented but have nagging pain or persistent symptoms, get evaluated within 72 hours. This is where Aptiva fits: we can image you (X-ray on site and MRI nearby), examine you, and get you started on a treatment plan the same day.
Document everything from the start. Take photos of the vehicles, the scene, and any visible injuries. Get the other driver's insurance information. Save the police report number.
Call your auto insurance carrier to notify them of the accident.
Seek medical attention right away. If you are in a serious accident or have concern for serious injury, go to the emergency department. Otherwise, call Aptiva Health (1-866-439-6704) or schedule your follow up visit after discharge from the emergency department with Aptiva Health.
Common Injuries Related to Auto Accidents
Car accidents produce a fairly predictable set of injuries depending on impact direction, speed, seatbelt use, airbag deployment, and the patient's age and prior health. The injuries below are the ones we evaluate and treat most often at Aptiva.
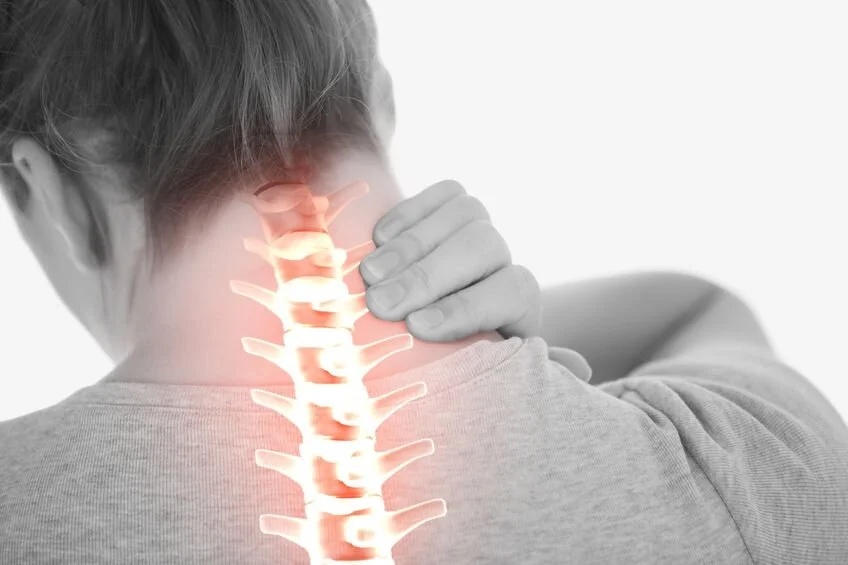
Whiplash and neck injuries
Whiplash-associated disorders are among the most common injuries following motor vehicle accidents, particularly in rear-end and side-impact collisions where rapid acceleration–deceleration forces are transmitted through the cervical spine. This sudden motion can lead to soft tissue strain of the neck muscles and ligaments, as well as more serious structural injuries such as cervical disc herniation and nerve root irritation (radiculopathy). Clinical studies have shown that a significant proportion of patients experience neck pain, stiffness, headaches, and radiating arm symptoms in the days to weeks following a crash, with some developing persistent or chronic symptoms if not treated early. Imaging and biomechanical research demonstrates that these forces can place abnormal stress on the intervertebral discs and facet joints, contributing to inflammation and nerve compression. Early evaluation and appropriate management including: physical therapy, guided rehabilitation, and when necessary advanced imaging or interventional care, are important to relieve symptoms, restore function, and reduce the risk of long-term complications.
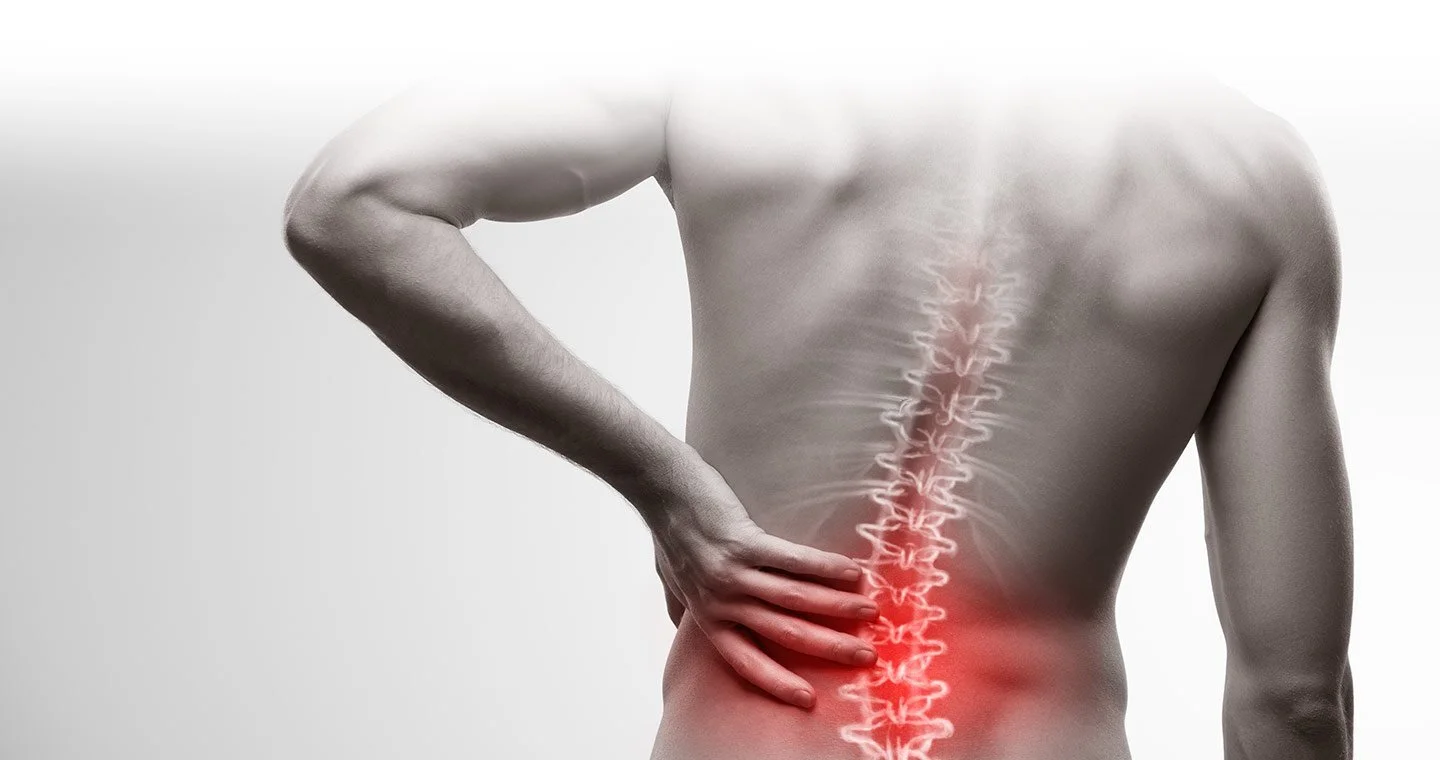
Back pain and lumbar injuries
Motor vehicle accidents are a well-documented cause of lumbar spine injuries, including low back pain, muscle strains, herniated discs, and sciatica, due to the significant forces transmitted through the lower spine during impact. Biomechanical research shows that crash forces can subject the lumbar spine to axial compression and flexion loading, which increases the risk of structural injury to vertebrae and intervertebral discs. Clinical studies further demonstrate that disruption of the intervertebral disc, such as tearing of the annulus fibrosus, can allow disc material to protrude and compress nearby nerve roots, leading to radiculopathy and radiating leg pain (sciatica). Traumatic lumbar disc herniation has been specifically identified in the literature as a consequence of high-energy events, including motor vehicle collisions. Additionally, imaging studies confirm that herniated discs and facet joint pathology are among the most common causes of low back pain and sciatica following injury. Early evaluation is important, as these injuries may not be immediately apparent but can lead to persistent pain, nerve symptoms, and functional impairment if left untreated.
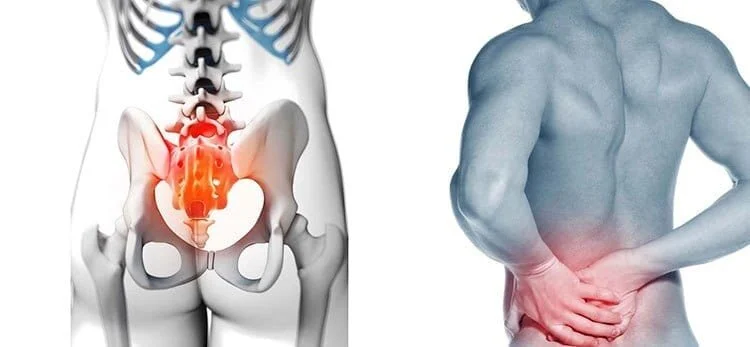
sacroiliac (SI) Joint Dysfunction
Side-impact (“T-bone”) collisions are a well-recognized mechanism for sacroiliac (SI) joint dysfunction, due to the lateral transfer of force through the pelvis at the time of impact. Published biomechanical and clinical studies have shown that asymmetric loading, especially when a vehicle is struck from the side, can create rotational and shear forces across the SI joints, leading to ligament strain, joint inflammation, and altered pelvic stability. Patients often present with low back, buttock, or hip pain that may mimic lumbar spine pathology but originates from the SI joint. Research suggests the SI joint may be a pain generator in 15–30% of patients with persistent low back pain after motor vehicle collisions, and the risk may be higher in side-impact crashes due to the directional force involved. Early recognition is important, as targeted treatments such as physical therapy, manual stabilization techniques, and image-guided injections can significantly improve outcomes and help prevent chronic dysfunction.
Concussion and head injuries
Motor vehicle accidents are a common cause of concussions and mild traumatic brain injuries (mTBI), even in the absence of a direct blow to the head. Studies show Rapid acceleration–deceleration forces during a crash can cause the brain to move within the skull, leading to a temporary disruption in normal brain function. These injuries often result in symptoms such as headaches, dizziness, confusion, memory difficulties, and sensitivity to light or noise, which may appear immediately or develop over hours to days following the accident. Research shows that concussions are typically caused by functional and neurochemical changes in the brain rather than visible structural damage, meaning standard imaging may appear normal despite ongoing symptoms. Because even “mild” brain injuries can lead to persistent issues such as post-concussion syndrome, early evaluation and appropriate care are essential to support recovery and prevent long-term complications. For more information on symptoms, diagnosis, and treatment, visit our concussion resource page: Learn more about concussion care at Aptiva Health.
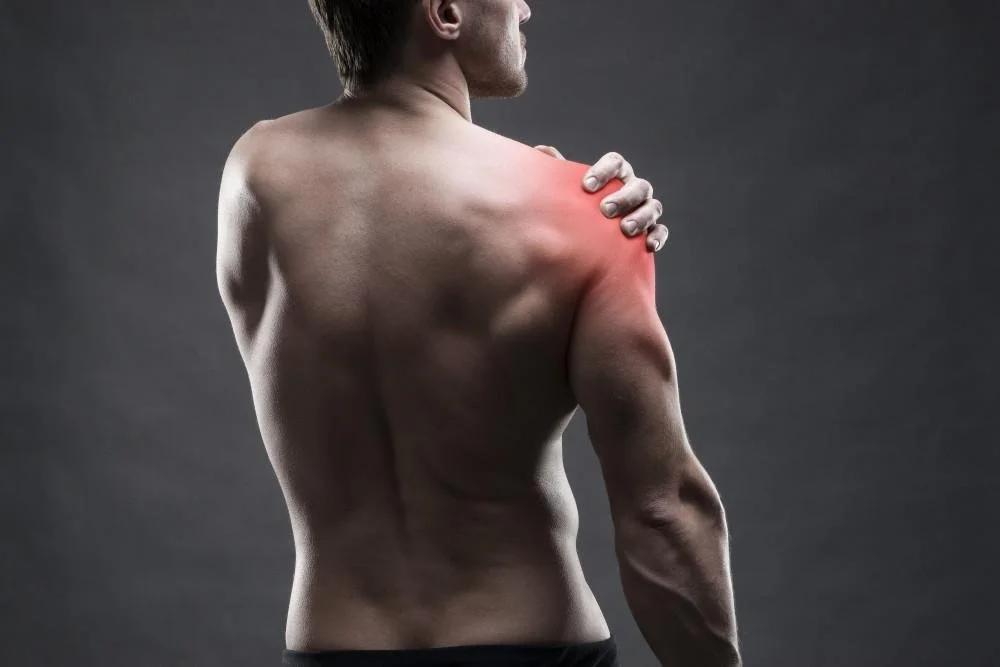
Shoulder injuries
Motor vehicle accidents are a common cause of shoulder injuries, including rotator cuff tears, labral tears, dislocations, fractures, and persistent shoulder pain, due to the significant forces transmitted through the upper extremities during impact. In a collision, occupants often brace against the steering wheel or seatbelt, which can place the shoulder in vulnerable positions and expose it to traction, compression, and rotational forces. Clinical literature shows that traumatic events can lead to rotator cuff tears and labral injuries, particularly when the arm is forcefully displaced or subjected to sudden loading. Shoulder dislocations, especially anterior dislocations, are also frequently associated with trauma and can damage surrounding soft tissues, including the labrum and stabilizing ligaments. In more severe cases, high-energy impacts such as motor vehicle collisions can result in fractures of the clavicle, proximal humerus, or scapula. These injuries may present with pain, weakness, reduced range of motion, and instability, and early evaluation is important to ensure proper diagnosis and treatment, reduce long-term dysfunction, and support full recovery.
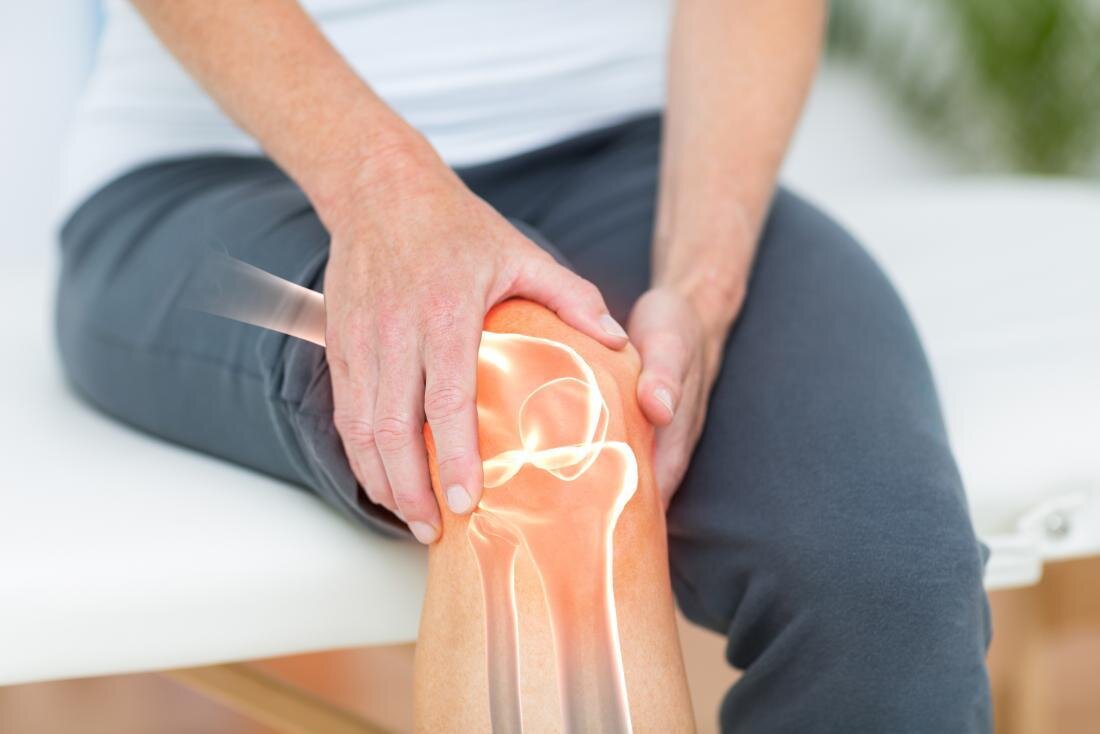
Knee injuries
Motor vehicle accidents are a common cause of knee injuries, including ligament tears (ACL, PCL, MCL), meniscal tears, fractures, and chronic knee pain, due to the forces transmitted through the lower extremities during impact. In many collisions—particularly frontal crashes—the knee may strike the dashboard, creating a “dashboard injury” mechanism that drives the tibia backward and places significant stress on the posterior cruciate ligament (PCL) and surrounding structures. Clinical literature shows that traumatic forces can result in ligament disruption, cartilage damage, and meniscal injury, leading to pain, swelling, instability, and difficulty bearing weight. High-energy trauma such as motor vehicle collisions is also a recognized cause of tibial plateau fractures and other intra-articular injuries, which can have long-term consequences if not properly treated. Because some knee injuries may not be immediately apparent after an accident, early evaluation and appropriate imaging are important to ensure accurate diagnosis, guide treatment, and prevent chronic instability or degenerative changes.
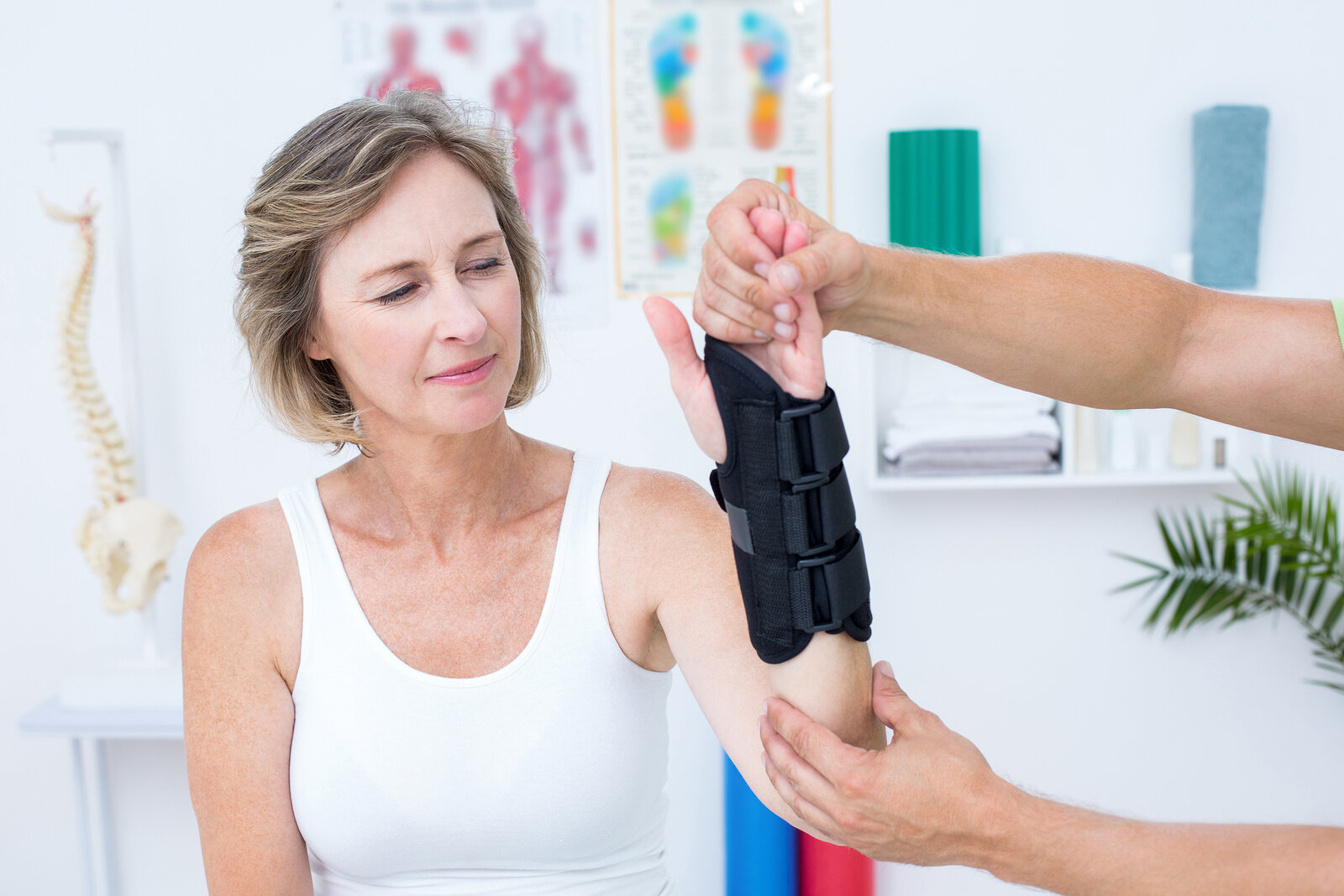
Wrist, hand, and elbow injuries
Motor vehicle accidents frequently cause wrist, hand, and elbow injuries, including fractures, ligament sprains, tendon injuries, and nerve compression syndromes, due to the instinctive bracing response during impact. Occupants often extend their arms against the steering wheel or dashboard, exposing the upper extremities to axial loading, hyperextension, and rotational forces. Clinical literature shows that this mechanism can result in common injuries such as distal radius (wrist) fractures, scaphoid fractures, and ligamentous injuries of the wrist and hand, which may lead to pain, swelling, and reduced grip strength. Elbow injuries including: dislocations, radial head fractures, and soft tissue strains, are also frequently associated with trauma and can significantly limit arm function. In some cases, patients may develop nerve-related symptoms such as numbness, tingling, or weakness, particularly if swelling or structural injury places pressure on surrounding nerves. Early evaluation is important, as certain injuries (such as scaphoid fractures or ligament tears) may not be immediately obvious but can lead to long-term complications if left untreated.
Musculoskeletal injuries, strains & sprains
Motor vehicle accidents commonly result in musculoskeletal injuries, including strains and sprains affecting muscles, ligaments, and tendons, due to the sudden forces placed on the body during impact. Rapid acceleration–deceleration and rotational movements can overstretch or tear soft tissues, leading to pain, stiffness, swelling, and reduced mobility in areas such as the neck, back, shoulders, and extremities. Clinical literature defines sprains as injuries to ligaments and strains as injuries to muscles or tendons, both of which are frequently caused by trauma and overloading of tissues beyond their normal range. These injuries may not always be immediately apparent after an accident but can worsen over time as inflammation develops. Research also shows that soft tissue injuries are among the most common outcomes of motor vehicle collisions, particularly in lower-speed crashes where structural damage may be limited but soft tissue stress is significant. Early evaluation and appropriate treatment including: physical therapy, guided rehabilitation, and activity modification, are important to promote healing, restore function, and reduce the risk of chronic pain or long-term impairment.
Mental, psychological & emotional impact
Motor vehicle accidents can result not only in physical injuries but also significant mental, psychological, and emotional trauma, including post-traumatic stress disorder (PTSD), anxiety, depression, and acute stress reactions. The sudden and often life-threatening nature of a crash can trigger lasting changes in how the brain processes fear and stress. Clinical research shows that a meaningful percentage of accident survivors develop PTSD symptoms such as intrusive memories, nightmares, hypervigilance, and avoidance behaviors, with some studies reporting rates around 10% or higher within the first year after a collision. In certain populations, rates can be even higher. One study found that up to 46% of crash victims met criteria for PTSD shortly after the event, with many also experiencing coexisting depression. Larger systematic reviews further confirm that individuals injured in motor vehicle crashes experience significantly elevated psychological distress, including depression and anxiety, which may persist for years after the accident. These emotional and cognitive effects can interfere with daily life, work, sleep, and the ability to drive or travel comfortably. Because psychological injuries are often less visible but equally impactful, early recognition and appropriate care, including counseling, cognitive behavioral therapy, and supportive medical management, are essential for recovery and long-term well-being.
Our Indianapolis Treatment Team
Frequently Asked Questions About Auto Injury Treatment in Indianapolis
Should I see a doctor after a car accident even if I feel fine?
Yes, typically within 72 hours. Whiplash, concussion, and soft-tissue injuries frequently don't always produce symptoms until 24 to 72 hours after the impact. Early evaluation rules out serious injury, starts treatment before chronic patterns develop, and creates the medical documentation that's important for any insurance claim.
Do I need a referral to be seen at Aptiva for a car-accident injury?
No. You can schedule directly without a referral. We can also accept physician referrals and walk-ins at locations with immediate injury care.
Does Aptiva accept MedPay coverage?
Yes. We accept and bill MedPay coverage. We also accept most insurances and can work with patients to make sure insurance coverage is not an issue.
How long does whiplash take to heal?
Most whiplash injuries improve substantially within 4 to 6 weeks of consistent physical therapy. A smaller percentage of patients have symptoms that persist beyond 3 months and may need imaging, interventional pain procedures, or — rarely — surgical evaluation.
Can Aptiva diagnose a concussion?
Yes. Our Concussion Team is one of the most experienced concussion programs and was awarded the Best in Class award in 2026. We utilize ImPACT neurocognitive testing and a structured return-to-activity protocol. Our neuropsychologists perform formal cognitive assessment for patients with persistent symptoms.
What if my injuries get worse weeks after the accident?
Come in. Symptoms that emerge or worsen weeks after an accident are common and treatable, but they need to be documented and evaluated promptly. Late-presenting symptoms are a normal part of recovery, not a reason to assume nothing is wrong.
Can I switch to Aptiva if I've already been seeing another provider?
Yes. We accept transfer-of-care from other providers. Bring your prior records, imaging, and PT notes and we'll integrate them into your plan.
Does Aptiva treat pediatric car-accident injuries?
We see adolescents and teenagers; younger pediatric patients should typically be evaluated through a pediatric-specific program first. Call us if you're not sure.